We’re pleased to announce that Pain Physicians of Wisconsin is now Pro Spine Pain.
We’re pleased to announce that Pain Physicians of Wisconsin is now Pro Spine Pain.
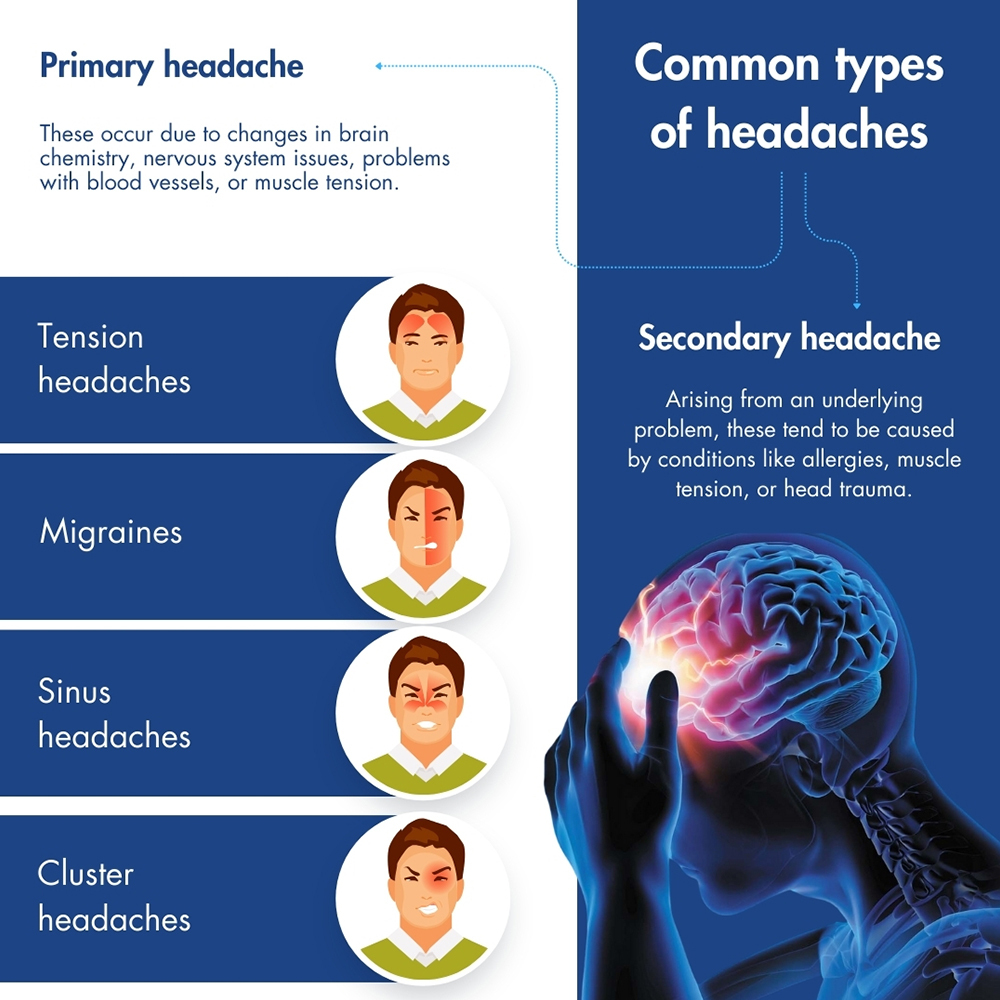 Headaches are a widespread and often debilitating health concern, affecting millions of individuals worldwide on a daily basis. They can manifest in various forms, including tension headaches, migraines, cluster headaches, and sinus headaches, each presenting with distinct symptoms and triggers.
Headaches are a widespread and often debilitating health concern, affecting millions of individuals worldwide on a daily basis. They can manifest in various forms, including tension headaches, migraines, cluster headaches, and sinus headaches, each presenting with distinct symptoms and triggers.
While tension headaches typically result from stress, poor posture, or muscle tension, migraines are characterized by intense throbbing pain, often accompanied by nausea, sensitivity to light, and sound. Cluster headaches occur in cyclical patterns and cause severe, excruciating pain around one eye or temple. Sinus headaches typically stem from sinus infections or allergies, leading to pressure and pain around the forehead, cheeks, and eyes.
Regardless of the type, headaches can significantly impair daily functioning, necessitating proper diagnosis by a headache specialist and management strategies tailored to your individual needs.
Headaches fall into two categories:
Headache symptoms can vary widely depending on the underlying cause.
Here’s a breakdown of symptoms for some of the most common types of headaches:
Each type of headache presents with its unique set of symptoms, which can greatly impact an individual’s daily life and functioning. Proper diagnosis and understanding of these symptoms are crucial for effective management and treatment of headaches. The pain management specialists at Pro Spine & Pain are available at five locations across Wisconsin to get to the bottom of your headaches and resolve your discomfort fast.
Headaches are a common ailment that affects people of all ages and backgrounds. While occasional headaches can be managed with simple remedies, recurring or severe headaches can impact your quality of life considerably. By understanding the risk factors associated with headaches, you can take steps to prevent their occurrence or reduce their intensity.
The following risk factors are most commonly associated with headaches:
Notably, recent migraine research has found that they are largely influenced by biological factors, with genetics and environmental elements playing significant roles in their development. Two studies indicate that around 50% of migraine risk is attributable to genetics.
Treating headaches involves various approaches tailored to the specific type and underlying cause of the headache.
To manage headaches caused by tension, over-the-counter pain relievers like acetaminophen or ibuprofen can often provide relief. Stress management techniques such as relaxation exercises, mindfulness, and regular exercise may also help alleviate tension headache symptoms.
For migraines, headache medications such as triptans or preventive drugs prescribed by a primary care physician can be effective in reducing the frequency and severity of attacks. Lifestyle modifications, including identifying and avoiding triggers such as certain foods, stress, or lack of sleep, can also play a crucial role in migraine management.
In cases of cluster headaches, prescription medications such as sumatriptan or oxygen therapy may be recommended to alleviate pain during an episode. Additionally, keeping a headache diary to track symptoms, triggers, and treatment effectiveness can assist in identifying patterns and optimizing management strategies.
In diagnosing the cause of your headaches, your physician may employ diagnostic equipment, such as CT scans and electroencephalography (EEG).
In severe cases that do not respond to less invasive treatment, you may be recommended therapeutic Botox® injections, nerve blocks, trigger point injections, or baclofen therapy (a muscle relaxant to address tension headaches).
Contact Pro Spine & Pain now to book a consultation with a pain expert with training in headache management for proper diagnosis and individualized treatment for your headaches.
If you experience occasional headaches, over-the-counter pain medication is usually effective and resolves the discomfort within 48 hours. However, if your headache persists beyond two days or occurs frequently, such as 15 days a month for three consecutive months, it’s advisable to seek evaluation at your local Pro Spine & Pain clinic.
You should also consider visiting the clinic if you have a headache after a head injury, if your headaches disrupt daily activities, if they don’t respond to over-the-counter medications, or if they cause severe pain. Additionally, seek immediate medical attention if your headache is accompanied by confusion, nausea, vomiting, dizziness, blurry vision, or fever.
For support and self-help guidelines, the National Headache Foundation website has some useful information to help you understand and deal with various types of headaches. For migraine-specific resources, we recommend the American Migraine Foundation website.
For specialized care and personalized treatment plans to address debilitating or chronic headaches, consider visiting the Pro Spine & Pain pain management clinic. Our expertise ensures comprehensive evaluation and effective relief, improving your overall well-being so you can get back to your regular activities.

Thomas Stauss, MD, completed both his undergraduate and medical studies at the esteemed University of Wisconsin in Madison. Dr. Stauss values having access to a wide array of cutting-edge treatment options, ensuring effective relief for his patients' discomfort and a significant enhancement in their quality of life. More specifically, he specializes in utilizing implanted devices to manage chronic pain. Dr. Stauss’s primary objective is to uphold the dignity of each patient while delivering ethical and professional services.
More about Dr. Stauss